TL;DR: Menopausal hormone therapy tracked with a 44.59% improvement in mood-symptom scores after about 107 days, across both peri- and postmenopausal women — and the gains were broadly similar regardless of which hormonal regimen was used.
Key Findings
- 44.59% improvement in mood symptoms: After initiating or optimizing menopausal hormone therapy, Meno-D mood-symptom scores decreased 44.59% (95% CI −46.83% to −42.34%, p < 0.001) over an average 107-day follow-up, meaning fewer reported symptoms.
- Both menopausal stages improved: Peri- and postmenopausal women showed similar gains — the signal wasn’t confined to the fluctuation-heavy perimenopause window.
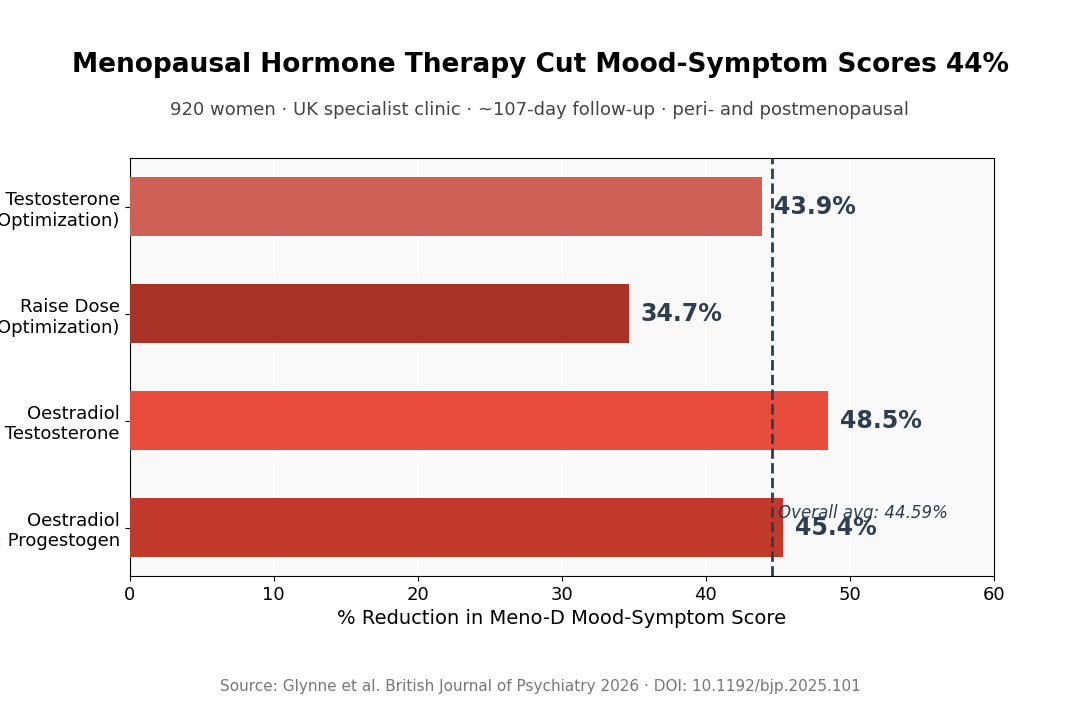
- Adding testosterone didn’t clearly separate: Women starting oestradiol ± progestogen improved 45.38%; those also starting testosterone improved 48.53% — a non-significant difference (p = 0.47).
- Optimization strategies were broadly equivalent: Higher oestradiol alone (34.70%), added testosterone (43.93%), or both together (43.25%) didn’t significantly diverge (p = 0.38).
- Multiple mood dimensions improved: Gains appeared across Meno-D’s individual items — low mood, anxiety, sleep, concentration, confidence — not just a single composite signal.
- Real-world clinic cohort, not a trial: 920 women from the UK’s largest specialist menopause service; observational design, no placebo, so expectancy and regression to the mean can’t be fully ruled out.
Source: The British Journal of Psychiatry (2026) | Glynne et al.
The public conversation about menopause is mostly vasomotor: hot flashes, night sweats, disrupted sleep. Mood symptoms get acknowledged — but usually as ambient background noise rather than the central problem. This is wrong for a lot of women, and this study reflects that.
For many people presenting to menopause clinics, low mood, anxiety, irritability, cognitive fog, and lost confidence are why they came — not a side effect of something more important. This retrospective cohort from the UK’s largest specialist menopause service took that psychiatric burden seriously and tracked what happened to it with treatment.
The Meno-D Scale Captured What Standard Questionnaires Often Miss
Most depression and anxiety scales weren’t designed with the menopausal transition in mind. The Meno-D questionnaire was. It captures symptoms specifically relevant to the menopause window: low mood, anxiety, sleep disruption, cognitive symptoms, reduced confidence, and changes in libido and energy.
Using a scale built for the population matters because a tool optimized for a different context will under-measure what’s actually changing. The authors deployed it clinic-wide, which is why the cohort reached 920 women — 448 perimenopausal and 435 postmenopausal.
The average follow-up was 107 days. That’s long enough to move past the first-week novelty effect but short enough to leave durability over years an open question.
A 44% Symptom Improvement Is Too Large to Dismiss as Noise
Average Meno-D mood-symptom scores decreased 44.59% after hormone therapy initiation or optimization. On this scale, lower scores mean fewer reported symptoms, so the change points toward improvement rather than worsened mood. The confidence interval was tight (−46.83% to −42.34%) and the p-value was far below conventional thresholds. That’s a large signal for a messy real-world dataset.
Observational study caveats apply — no randomization, no placebo, no blinding. Regression to the mean, expectancy, and close specialist follow-up can all inflate an apparent treatment effect. But a nearly 45% symptom reduction across 920 women is a number that would be meaningful even after those discounts are applied.
The broader finding — that both peri- and postmenopausal women improved — matters clinically. The common assumption is that hormones help mainly during perimenopause, when estrogen is actively fluctuating. This cohort suggests the mood benefit may persist into postmenopause, which broadens the population for whom hormone therapy might be considered for psychiatric symptoms.
Testosterone Did Not Emerge as a Clear Mood Advantage
One of the live clinical debates in menopause care is whether adding testosterone to estradiol provides a special edge for mood and cognitive symptoms. This cohort gives a fairly restrained answer: not detectably, at least not at the group level.
At treatment initiation, women starting oestradiol with or without progestogen improved 45.38%; those who also started testosterone improved 48.53%. That’s a 3-point difference in the expected direction, but it didn’t reach statistical significance (p = 0.47). Similar null results appeared across the optimization strategies tested.
That’s not a case against testosterone — the study wasn’t powered to detect small differences between hormone regimens, and individual women may still respond differently. But it does challenge the narrative that testosterone is the essential missing piece for mood. The data suggest that oestradiol-based treatment already does a lot of the work.
Progestogen Type Did Not Drive the Mood Outcome
The cohort included different progestogen strategies — body-identical progesterone and the levonorgestrel IUS — without a major mood difference emerging between them. That’s reassuring for patients who worry that their progestogen choice will undercut the mood benefit of oestradiol.
It also makes the study more generalizable. Menopause services don’t prescribe a single regimen; they adjust based on preference, contraindications, prior history, and individual response. Finding consistent mood improvements across varied strategies is more clinically useful than a result that applies only to one specific combination.
Hormones Belong in the Psychiatric Differential for Perimenopausal Women
The paper stops well short of saying hormone therapy should replace antidepressants or psychotherapy for menopausal mood disorders. That’s appropriate caution. Menopausal depression and anxiety are heterogeneous — some women will still need psychiatric-focused treatment regardless of hormonal status.
But the implication is clear: in the menopausal window, hormones aren’t just context for psychiatric symptoms. They’re a plausible treatment target. A 44% reduction in mood-symptom burden over a clinic follow-up is too substantial to treat as incidental.
The clinical default — manage mood with antidepressants while treating menopause symptoms separately — misses an opportunity. For women presenting with low mood, anxiety, and cognitive fog alongside hot flashes or cycle changes, addressing the hormonal substrate earlier rather than later makes biological sense.
What this study can’t answer is durability. Three and a half months of follow-up shows the treatment is moving in the right direction; it doesn’t tell us whether the mood benefit persists at one or two years. That’s the next critical measurement.
Citation: Glynne et al. Transdermal oestradiol and testosterone therapy for menopausal depression and mood symptoms: retrospective cohort study. The British Journal of Psychiatry. 2026;228(5):429–436. DOI: 10.1192/bjp.2025.101
Study Design: Retrospective cohort study at a specialist UK menopause clinic.
Sample Size: 920 women (448 perimenopausal, 435 postmenopausal); average follow-up 107 days.
Key Statistic: Meno-D mood-symptom scores decreased 44.59% (95% CI −46.83% to −42.34%, p < 0.001) after hormone therapy initiation or optimization.