TL;DR: Routine MS monitoring focuses on the brain — but prior data suggest 12% of new spinal cord lesions appear with no simultaneous brain activity. The MSpine trial is now testing whether systematic whole-spine MRI catches disease that standard follow-up is missing.
Key Findings
- 31.2% of spinal lesions may be asymptomatic: Prior retrospective data suggest nearly a third of new cord lesions produce no symptoms, meaning symptom-triggered imaging misses them entirely.
- 12.1% arise with no concurrent brain activity: A meaningful fraction of cord lesions appear even when brain MRI looks stable — the current monitoring backbone could be missing active disease.
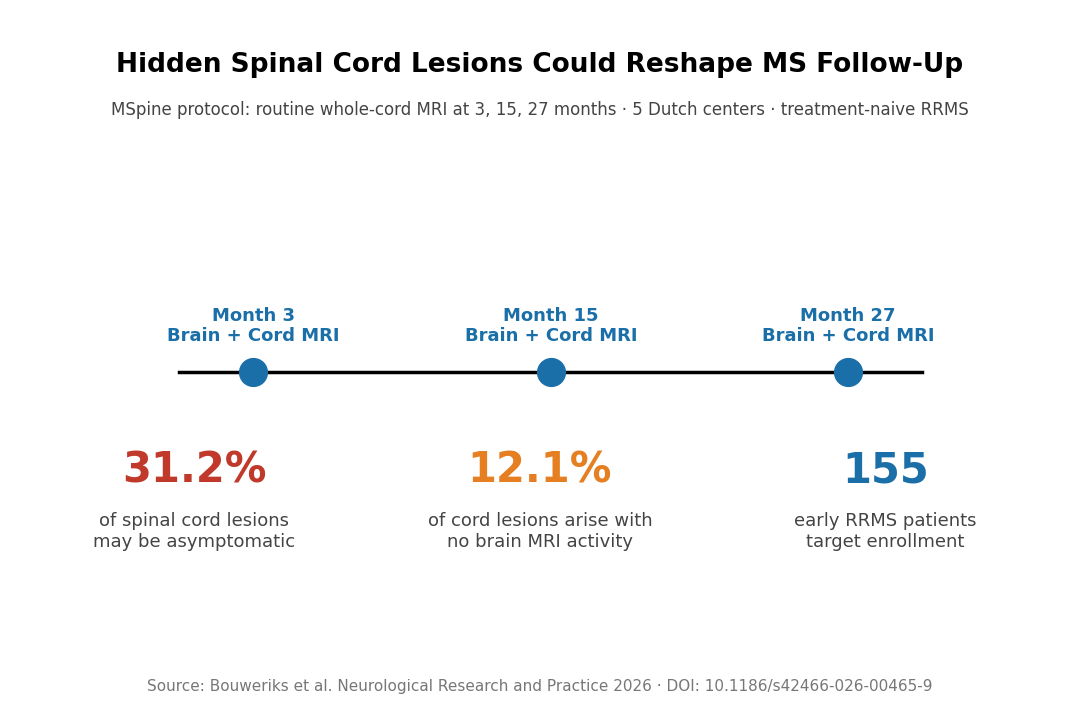
- MSpine will add whole-cord MRI at 3, 15, and 27 months: Target enrollment is 155 treatment-naive RRMS patients starting their first disease-modifying therapy within 5 years of onset.
- The key output is a number-needed-to-scan: Rather than asking if more imaging is better in theory, the trial calculates how many patients need routine spinal MRI to catch one case of otherwise hidden disease.
- Biomarkers will help identify cord-predominant patients: Blood markers (NfL, GFAP), CSF data where available, lymphocyte subsets, immune checkpoint markers, and lesion location will test whether imaging can be targeted to those most likely to benefit.
- Protocol paper — no efficacy results yet: This is a study design publication; the clinical findings will come from the completed trial.
Source: Neurological Research and Practice (2026) | Bouweriks et al.
There’s a structural blind spot in how multiple sclerosis is monitored. Brain MRI is the backbone of routine follow-up — it’s the tool that defines treatment response, guides escalation decisions, and fills out disability-progression metrics. The spinal cord gets imaged mainly when symptoms point there.
That asymmetry has a practical justification: spinal MRI is slower, technically demanding, and harder on scanner capacity. But it sits uneasily with everything the field knows about disability in MS. Cord lesions drive walking problems, hand dysfunction, and bladder symptoms — the outcomes that actually shape patients’ lives. Yet the monitoring framework was built around the brain.
The MSpine protocol exists because that default may be costing clinicians information they need.
A Third of Cord Lesions Are Silent, and 12% Appear Without Brain Activity
The protocol cites two striking numbers from prior retrospective data: roughly 31.2% of new spinal cord lesions are asymptomatic, and 12.1% arise independently of simultaneous brain MRI activity.
The 12% figure is the more clinically consequential one. It means that using brain MRI as the primary disease-activity monitor will miss about 1 in 8 new cord lesions — not because imaging technology is limited, but because the cord isn’t being imaged. A patient could be classified as “stable” on standard follow-up while silently accumulating spinal inflammatory activity.
This matters most in early disease, when treatment decisions are being made. Escalating therapy requires evidence of active disease. If cord activity isn’t captured, those escalation triggers may be missed — and early treatment windows, when the disease is most responsive, may be underused.
MSpine Will Turn Routine Spinal MRI From Troubleshooting Into Surveillance
The key design choice in MSpine is deliberately ambitious: whole-cord MRI becomes scheduled rather than symptom-triggered. At approximately 3, 15, and 27 months, participants will get complete sagittal and axial spinal cord imaging alongside their routine brain scan.
The enrolled population — 155 treatment-naive relapsing-remitting patients starting their first disease-modifying therapy — is chosen for clinical relevance. These are people in whom a hidden lesion could directly alter decisions about which drug to use, how long to wait before escalating, and whether current treatment is working.
Images will be read locally for clinical care and then reviewed centrally to test inter-rater reliability. That combination matters: a monitoring change only scales if the imaging findings are reproducible enough to guide real decisions in different settings.
The Number-Needed-to-Scan Makes This a Healthcare Decision Tool
Most monitoring studies end with “more imaging found more lesions.” MSpine is structured around a more practical question: how many patients need routine spinal imaging to catch one case of clinically important hidden disease activity that would have been missed?
That framing matters for health systems. Adding a scan to every follow-up visit is only defensible if the yield — measured in treatment changes, not just lesion counts — justifies the cost and burden. A concrete number-needed-to-scan is the kind of metric that neurologists, radiologists, and payers can use to decide whether the change is worth making.
If the answer is “image 5 patients to catch 1 case of hidden active disease that alters management,” that’s a compelling argument for routine cord surveillance. If it’s “image 50 patients,” the answer is probably a targeted approach based on risk stratification rather than universal screening.
Biomarkers Will Help Target the Right Patients
Even if routine cord MRI proves its value, scanning every MS patient indefinitely may not be efficient. The protocol’s biomarker arm addresses this: by correlating spinal lesion activity with blood markers like neurofilament light chain (NfL) and GFAP, CSF findings where available, lymphocyte subset profiles, immune checkpoint markers, and presenting syndrome, the investigators want to identify a subgroup in whom cord-predominant disease is most likely.
That’s where this moves from an imaging audit to a precision monitoring question. The goal isn’t “scan everyone more” — it’s “learn who needs routine cord imaging because that’s where their disease declares itself, and spare the others.”
If a cord-predominant patient subtype can be identified using accessible blood markers, it becomes possible to triage: routine brain-plus-cord imaging for those at elevated spinal risk, brain-focused monitoring for those whose disease activity is predominantly cerebral. That kind of stratification would make the intervention both more useful and more scalable.
A Protocol Paper That Points at a Genuine Gap
No efficacy results appear here — this is the study design, not the findings. Protocol papers matter when they’re addressing a question the field has quietly accepted without rigorous testing. MS monitoring has been brain-centric by habit more than by evidence.
The study also touches newer frameworks. Concepts like PIRA — progression independent of relapse activity — and PIRMA — MRI activity without matching symptoms — both suggest that current monitoring may systematically undercount disease activity. Hidden spinal lesions are a plausible contributor to those puzzling patterns.
If MSpine finds substantial independent cord activity, the implication isn’t just adding a scan. It’s that the definition of “stable MS” may need revision. Treatment-escalation algorithms built around brain MRI may be systematically underreacting to active disease in one of the most clinically important compartments of the nervous system.
Citation: Bouweriks et al. MSpine: a prospective longitudinal study of spinal cord lesions in multiple sclerosis: MRI monitoring and prognostic factors for active disease. Neurological Research and Practice. 2026;8:23. DOI: 10.1186/s42466-026-00465-9
Study Design: Prospective multicenter study protocol; 5 Dutch MS centers.
Sample Size: 155 treatment-naive RRMS patients (target enrollment), aged 18–65, starting first disease-modifying therapy within 5 years of onset.
Key Statistic: Prior data: 31.2% of spinal cord lesions may be asymptomatic; 12.1% may arise without concurrent brain MRI activity.