TL;DR: A 2026 Psychological Medicine network meta-analysis of 26 randomized trials found AVATAR therapy matched CBT immediately after treatment and outperformed it at 3 months for auditory hallucination severity, with fewer sessions.
Key Findings
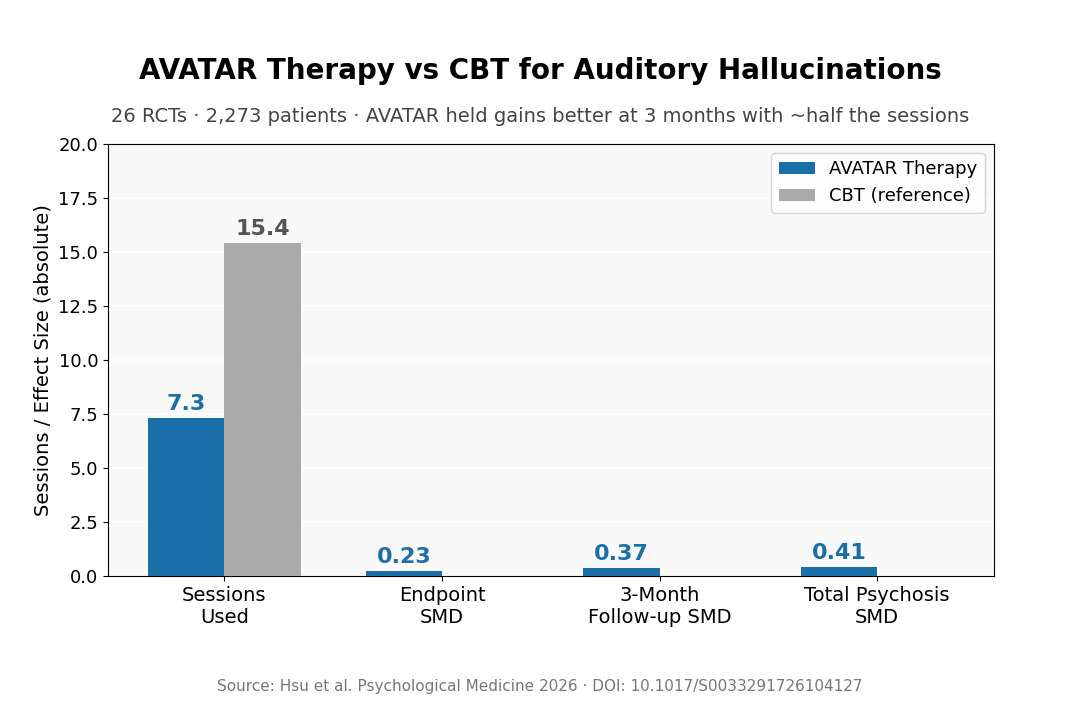
- No clear edge at treatment end: AVATAR did not significantly beat CBT on voice severity right after therapy ended (SMD = −0.23, 95% CI −0.55 to 0.10) — though it ranked best across the network overall.
- 3-month durability favored AVATAR: After sessions stopped, AVATAR held its gains better than CBT (SMD = −0.37, 95% CI −0.69 to −0.05) — the therapy faded less.
- Total psychosis scores moved more: AVATAR also outperformed CBT on overall psychotic symptom burden (SMD = −0.41, 95% CI −0.75 to −0.06), not just voice severity.
- 7.3 sessions versus 15.4: AVATAR protocols used about half as many sessions as CBT, raising the question of whether the efficiency advantage could survive larger trials.
- Mood, anxiety, and quality of life did not separate: AVATAR showed no clear edge over CBT on depression, anxiety, negative symptoms, or broader functioning.
- Bias and small-study effects cloud the picture: Most trials carried moderate-to-high risk of bias, Egger’s tests flagged small-study effects, and AVATAR’s evidence base (396 participants) was smaller than CBT’s (824).
Source: Psychological Medicine (2026) | Hsu et al.
Persistent auditory hallucinations are one of psychiatry’s most treatment-resistant problems. Antipsychotics help many patients, but the voices often survive — quieter, maybe, but still there.
The default non-drug answer has been CBT for psychosis, which has guideline support but asks a lot: conceptual reframing, sustained engagement, and a therapeutic approach that can feel abstract when someone is carrying heavy symptom burden.
AVATAR therapy was built as a more concrete alternative.
Instead of coaching patients to think differently about the voice, it gives the voice a digital face and lets the therapist step between roles — speaking as the avatar, then speaking as themselves — until the patient learns to challenge and resist it in real time.
Ameta-analysis is the first systematic attempt to put AVATAR and CBT head to head across the available evidence.
26 Randomized Trials Compared AVATAR Therapy, CBT, and Other Treatments
Direct head-to-head comparisons between AVATAR and CBT are rare, so the authors used a network meta-analysis — combining direct and indirect evidence across 26 RCTs, 2,273 participants, and several comparators including psychoeducation, supportive therapy, social-activity therapy, and treatment as usual.
The sample was clinically realistic. Mean age was 39.3 years, about two-thirds were male, and most trials enrolled patients with schizophrenia-spectrum disorders who were stable on outpatient medication but still heard distressing voices. This is the persistent-voices population that fills community mental health caseloads: medicated, reasonably stable, but not well.
The study also wasn’t asking “which therapy beats doing nothing.” It was asking specifically whether AVATAR can outperform CBT for people whose voices have already survived medication.
At Treatment End, AVATAR and CBT Tracked Together
The endpoint comparison was not the decisive result the field might want. AVATAR’s advantage over CBT on hallucination severity at the end of treatment was numerically real (SMD = −0.23) but the confidence interval crossed zero, meaning the difference wasn’t statistically established. AVATAR ranked highest across the network on this outcome, but the evidence was too wide to call it a knockout.
That’s a point worth sitting with. Ranking first in a network isn’t the same as winning head-to-head. The uncertainty around AVATAR’s endpoint result comes partly from its smaller evidence base — 396 participants across 7 arms versus CBT’s 824 across 24.
The Durability Signal of AVATAR
Three months after treatment stopped is where AVATAR found its edge. On voice severity at follow-up, AVATAR held significantly better than CBT (SMD = −0.37, 95% CI −0.69 to −0.05). Statistically, that confidence interval barely avoids zero — but the direction was consistent, and it’s the kind of outcome that matters most clinically.
Most psychiatric treatments show their best numbers at discharge and then flatten. A therapy that continues to hold after sessions end is offering something different: not just a coping boost, but possibly a more durable shift in how the patient relates to the voice.
The mechanism behind the durability is plausible. AVATAR therapy puts the patient in an active confrontational stance toward the hallucination.
The voice gets externalized, argued with, and gradually disempowered over sessions. That kind of mastery might consolidate differently than CBT’s cognitive restructuring — especially for patients who struggle with abstract reasoning when symptom burden is high.
Total Psychosis Scores Moved Even When Anxiety and Mood Didn’t
AVATAR also outperformed CBT on overall psychotic symptom burden (SMD = −0.41), a result that suggests the benefit wasn’t limited to the voice itself. Something in the broader psychotic symptom load appeared to shift more with AVATAR.
That asymmetry is worth noting. Depression, anxiety, negative symptoms, and quality of life did not show a clear AVATAR advantage.
So this isn’t a broad-spectrum emotional therapy. The signal is relatively targeted: voice-related distress and total psychosis burden, with limited reach into mood or functioning domains.
For patients whose primary suffering is the voices themselves — and for whom CBT’s broader mood work is secondary — that specificity may actually be appropriate.
Efficiency Could Matter for Services
AVATAR protocols averaged 7.3 sessions in included trials versus 15.4 sessions for CBT. That doesn’t automatically mean AVATAR is more efficient, because longer treatments can achieve different things. But if similar or better durability is achievable in fewer sessions, the service-design implications are real — particularly in overburdened community mental health settings where waiting lists are long and therapy slots are limited.
The efficiency argument is speculative until confirmed in larger trials with a focus on health-system outcomes. But it’s one of the paper’s more actionable claims.
Small-Study Effects and Bias Keep the Verdict Provisional
Egger’s tests flagged significant small-study effects for both the primary hallucination outcome and the 3-month follow-up result. Most trials carried moderate-to-high bias risk. AVATAR’s evidence rests on substantially fewer patients than CBT’s.
There’s also a methodological nuance: CBT trials often target broader positive symptoms, while AVATAR trials are more specifically built around voice work. When the comparison groups aren’t aiming at exactly the same outcome, network estimates need extra scrutiny.
So the verdict should be calibrated, not enthusiastic. AVATAR looks genuinely promising.
It can be more efficient and the durability signal matters, but the research does not support replacing CBT with avatar therapy based on current evidence. That said, it supports treating AVATAR as a serious option worth testing in larger, better-powered trials.
Particularly interesting open questions: Can AVATAR be delivered remotely without losing the effect? Which patients benefit most — those with prominent voice distress, better cognitive engagement, fewer negative symptoms? And can it be delivered as a focused module inside broader psychosis care rather than as a standalone treatment?
This meta-analysis moves AVATAR out of the novelty bucket. It no longer looks like a clever tech-adjacent add-on. It looks like a plausible next-generation option for one of schizophrenia’s most persistent and disabling symptoms.
Citation: DOI: 10.1017/S0033291726104127. Hsu et al. AVATAR versus cognitive-behavioral therapy for medication-resistant auditory hallucination: a systematic review and network meta-analysis. Psychological Medicine. 2026;56:e107.
Study Design: Systematic review and network meta-analysis of 26 RCTs.
Sample Size: 2,273 adults with schizophrenia-spectrum disorders and medication-resistant auditory hallucinations.
Key Statistic: AVATAR vs CBT at 3-month follow-up: SMD = −0.37 (95% CI −0.69 to −0.05). Session count: 7.3 vs 15.4.