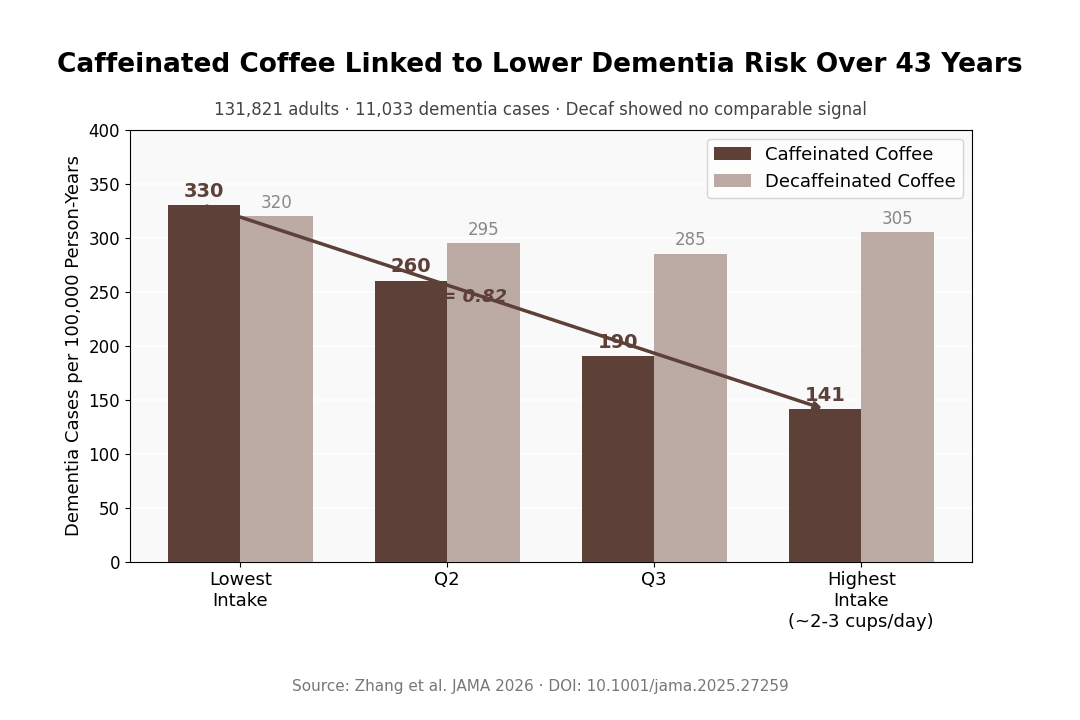
TL;DR: Caffeinated coffee drinkers had 141 vs 330 dementia cases per 100,000 person-years in the highest versus lowest intake quartiles — across 131,821 adults followed up to 43 years. Decaf showed no comparable signal.
Key Findings
- Caffeinated coffee: 141 vs 330 dementia cases per 100,000 person-years: Highest vs lowest intake quartile; adjusted hazard ratio 0.82 (95% CI 0.76–0.89).
- Decaffeinated coffee showed no comparable signal: The caffeine contrast separates a true beverage-habit effect from something specific to caffeinated consumption — though decaf drinkers may also differ in health status.
- Dose-response peaked at 2–3 cups/day: The strongest association appeared at moderate intake, not unlimited coffee — higher doses didn’t appear to add benefit and may introduce competing harms.
- Subjective cognitive decline: 7.8% vs 9.5%: Highest vs lowest caffeinated coffee quartile — a modest but directionally consistent signal across cognitive outcomes.
- Tea showed a similar pattern at 1–2 cups/day: Consistent with caffeinated coffee, tea intake was also associated with lower dementia risk at moderate levels.
- 131,821 participants, 11,033 dementia cases, up to 43 years follow-up: Nurses’ Health Study and Health Professionals Follow-Up Study combined; repeated dietary reports rather than a single baseline snapshot.
Source: JAMA (2026) | Zhang et al.
Coffee research in dementia has a credibility problem: coffee drinkers are healthier in other ways. They tend to be more educated, more physically active, less likely to smoke, and more engaged in professional and social life. A simple association between coffee and lower dementia risk could easily reflect who drinks coffee rather than what coffee does.
The Zhang et al. JAMA study went as far as an observational cohort reasonably can to address this. It combined two large US professional cohorts with up to 43 years of follow-up, used repeated dietary reports (not a single baseline snapshot), and separately analyzed caffeinated coffee, decaffeinated coffee, and tea. What emerged was specific enough to take seriously.
43 Years of Follow-Up Is the Right Scale for This Question
Dementia is a disease of decades. The brain changes that lead to Alzheimer’s and vascular dementia begin accumulating in midlife or earlier, long before any cognitive symptom appears. An exposure measured once at age 50 and linked to dementia at 75 or 80 is testing the right biological timeframe.
The Nurses’ Health Study (86,606 women, 1980–2023) and Health Professionals Follow-Up Study (45,215 men, 1986–2023) together provided exactly that: repeated dietary questionnaires collected every few years across a median follow-up of 36.8 years. That’s not “we asked people to recall their lifetime coffee habits at the time of diagnosis.” It’s decades of prospective tracking during the period when dementia risk was presumably accumulating.
With 11,033 incident dementia cases across the combined dataset, the study also had enough events to find real patterns rather than noise.
The Decaf Comparison Is the Study’s Most Informative Design Choice
The clearest scientific contribution here isn’t the hazard ratio for caffeinated coffee — it’s the contrast with decaffeinated coffee. Decaf showed no significant association with lower dementia risk.
This matters because the comparison helps separate two distinct explanations. If the dementia benefit were entirely driven by the kind of person who drinks coffee (healthier lifestyle, higher education, more social engagement), decaf drinkers should look similar — they share most of those characteristics. The fact that decaf doesn’t carry the same signal points toward something more specific about caffeinated intake.
The logical candidates are caffeine itself (adenosine-receptor blockade, neuroprotective signaling, vascular effects) or polyphenols and other bioactive compounds that are present in different amounts or forms in caffeinated versus decaffeinated coffee. The study can’t separate these mechanisms, but it narrows the exposure worth investigating.
The 2–3 Cup Sweet Spot Has a Biological Rationale
The dose-response curve is one of the more practically useful parts of the paper. The association between caffeinated coffee and lower dementia risk didn’t keep climbing with increasing dose. It peaked around 2–3 cups per day and flattened or attenuated beyond that. For tea, the strongest signal appeared at around 1–2 cups per day.
That plateau has a plausible biological interpretation. Caffeine blocks adenosine receptors, which can reduce neuroinflammation, improve cerebral blood flow, and modulate dopaminergic and cholinergic signaling — mechanisms with credible links to long-term neuroprotection. But high caffeine doses also disrupt sleep, raise cortisol, increase blood pressure in susceptible people, and worsen anxiety. Poor sleep is independently a dementia risk factor. So the dose-response curve may be the result of beneficial effects saturating at moderate intake while competing harms accumulate at higher doses.
The practical message is therefore not “drink as much coffee as possible.” It’s that moderate habitual intake appears to be the exposure that tracks with brain health benefit in these cohorts — not maximizing caffeine.
What This Doesn’t Prove
This was a prospective cohort study, not a randomized trial. Coffee drinkers differ from non-drinkers in many ways beyond just caffeine intake, and statistical adjustment can’t fully account for everything. Reverse causation is also possible — early subclinical dementia pathology could reduce coffee intake before any diagnosis is made, creating an apparent protective association.
The fact that the same professional cohorts (relatively highly educated, health-conscious, with good healthcare access) were used throughout also limits generalizability. The associations may not translate directly to other populations.
The right framing for anyone reading this is calibrated rather than prescriptive: for adults who already tolerate caffeinated coffee or tea, moderate habitual intake fits with a brain-healthy pattern in two very large prospective cohorts followed for decades. For people whose caffeine worsens sleep, anxiety, palpitations, or blood pressure, this study doesn’t override individual medical context.
The cleanest scientific question now is mechanism. Randomized trials of caffeine supplementation exist but tend to be short-term and small. What’s needed is a clearer map of which pathway — adenosine signaling, vascular health, inflammation, polyphenol metabolism — drives the long-term association. That would turn this finding from an association to a target.
Citation: Zhang et al. Coffee and Tea Intake, Dementia Risk, and Cognitive Function. JAMA. 2026;335(11):961–974. DOI: 10.1001/jama.2025.27259
Study Design: Prospective cohort study; Nurses’ Health Study and Health Professionals Follow-Up Study; repeated dietary reports.
Sample Size: 131,821 participants; 11,033 incident dementia cases; median follow-up 36.8 years (up to 43 years).
Key Statistic: Highest vs lowest caffeinated coffee quartile: 141 vs 330 dementia cases per 100,000 person-years; HR 0.82 (95% CI 0.76–0.89). Decaffeinated coffee: no significant association.