TL;DR: A 2026 randomized trial in The British Journal of Psychiatry found 6 ketamine infusions improved severe treatment-resistant depression, but curated music added no measurable benefit; higher mystical-experience scores still predicted the next session’s depression outcome.
Key Findings
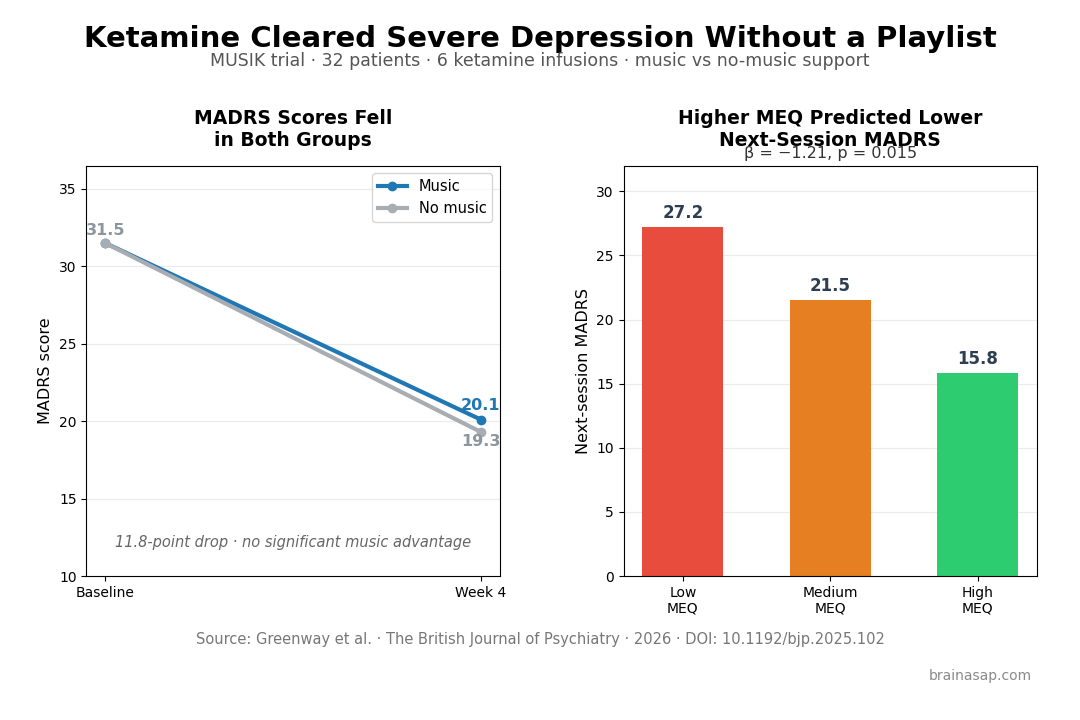
- MADRS fell 11.8 points by week 4: Scores dropped from 31.5 to 19.7 (d = 1.2, p < 0.001) across both groups — gains that held at week 8, 4 weeks after the last infusion.
- Music added nothing: Curated playlists produced no significant advantage over matched non-music support on depression, anxiety, suicidality, or psychedelic-experience scores.
- Mystical experience predicted next-session outcome: Higher Mystical Experience Questionnaire (MEQ) scores at one session predicted lower depression scores at the next (MADRS: β = −1.21, p = 0.015; BDI: β = −1.42, p = 0.004).
- Peak MEQ explained 35–49% of outcome variance at week 4: Adjusted R² = 0.356 for MADRS, 0.489 for BDI — the subjective altered-state quality was a strong predictor even in this heavily comorbid sample.
- Emotional breakthrough didn’t predict outcome after controlling for session number: Catharsis-type experiences rose across sessions but lost predictive power once the accumulation effect was controlled.
- Severe cohort, 81% with personality disorder, 78% with active suicidal ideation: 32 adults at two Montreal sites; 28 of 32 completed all planned visits; no serious adverse events.
Source: The British Journal of Psychiatry (2026) | Greenway et al.
Music has become part of the mythology around psychedelic and psychedelic-adjacent therapies.
The playlist rises, the mind opens, the treatment works. Ketamine clinics have absorbed this logic — rooms are softened, playlists are curated, and the soundtrack is sometimes treated almost like a therapeutic tool in itself.
The MUSIK trial from Montreal tested that assumption directly, and the data showed clear: the playlist didn’t add measurable psychiatric benefit.
But the part of the ketamine experience that did matter — the quality of the altered state itself — turned out to be a surprisingly strong predictor of what happened next.
MUSIK Trial Tested Ketamine Plus Curated Music in Severe TRD
MUSIK enrolled 32 adults with severe treatment-resistant depression. Mean MADRS score at entry was 31.5, which placed the group in the severe range.
The average Dutch Measure of Treatment Resistance score was 16.7. Most participants carried more than three psychiatric diagnoses: 81% had personality disorder; 78% had clinically significant suicidal ideation at baseline.
The baseline severity matters because the trial was not testing ketamine in a mild or low-comorbidity sample. It tested whether a supportive six-infusion protocol could reduce symptoms in patients who had already failed conventional treatment and were carrying unusually heavy clinical burden.
The protocol: six 40-minute IV infusions at 0.5 mg/kg over 4 weeks (2 sessions/week for weeks 1–2, then weekly), plus weekly one-hour psychotherapy for everyone, plus post-session discussion in both groups. The only difference between arms was the presence or absence of a curated music playlist.
Ketamine Improved MADRS Scores Without a Music Advantage
By week 4, MADRS scores had fallen from 31.5 to 19.7 — an 11.8-point drop and a large effect size (d = 1.2). BDI fell with d = 0.87, anxiety with d = 0.80. The durability at week 8 was meaningful: MADRS d = 1.2, BDI d = 0.97 at a point 4 weeks after the last infusion.
None of that separated by music condition. The music group and the no-music group improved in parallel, and no analysis — depression outcomes, anxiety outcomes, suicidality, MEQ scores, emotional breakthrough scores — showed a significant music advantage.
That null result is worth reading carefully. It doesn’t say context is irrelevant — both groups received a carefully supportive container: dimmed rooms, clinician presence, blindfolds, reassurance, post-session processing, and weekly therapy.
The non-music arm was never bare-IV ketamine. The comparison was music versus another active supportive condition.
The most precise conclusion is: a curated playlist added no psychiatric benefit over well-structured non-music support. Whether music helps compared to a truly bare clinical ketamine experience remains untested.
MEQ Scores Predicted Lower Next-Session Depression
The secondary predictor result came from subjective-experience ratings collected after each ketamine session. Researchers measured two types of experience: mystical-type experience (unity, transcendence, deep positive affect, ineffability) and emotional breakthrough (catharsis, the sense that difficult material opened up).
Emotional breakthrough scores rose across the treatment course — later sessions felt more emotionally significant. But once session number was controlled, emotional breakthrough no longer predicted the next session’s depression score.
Mystical-type experience held up differently. Higher MEQ scores at one session predicted lower depression scores at the next, even after accounting for accumulating treatment effect. At week 4, peak MEQ scores explained an adjusted R² of 0.356 for MADRS and 0.489 for BDI — a substantial proportion of outcome variance in a small sample.
That distinction changes interpretation. Catharsis-like emotional breakthrough did not independently predict later depression scores after session number was controlled. The broader mystical-type experience captured by the MEQ was the subjective measure that predicted the next-session outcome.
Ketamine Support May Matter Beyond a Specific Playlist
The practical message isn’t “turn off the music.” Clinics can keep playlists without worrying this study condemns them. But the playlist shouldn’t be mistaken for the therapeutic mechanism.
The more consequential implication is that the quality of the ketamine experience predicted treatment outcome beyond simple group assignment. The trial leaves causality open, but it makes subjective experience a measurable candidate predictor rather than background atmosphere.
For severely treatment-resistant patients, that distinction changes what future trials should measure. Dose, preparation, therapist support, room conditions, and post-session processing may be worth testing directly, while a specific curated playlist did not separate outcomes in MUSIK.
The sample was small (32 patients), the analysis of experiential predictors was secondary and exploratory, and expectation effects can’t be fully removed from subjective ratings. But the MEQ finding was large enough and consistent enough across outcome measures to warrant follow-up in larger, pre-registered trials.
The next trial should test which parts of the ketamine session predict later symptom change, without assuming that music is the active ingredient.
Citation: DOI: 10.1192/bjp.2025.102; Greenway et al; The Music for Subanesthetic Infusions of Ketamine randomized clinical trial: ketamine as a psychedelic treatment for highly refractory depression; The British Journal of Psychiatry; 2026;228:437–445.
Study Design: Randomized clinical trial; two Montreal sites.
Sample Size: 32 adults with severe treatment-resistant depression (81% personality disorder, 78% active suicidal ideation); 181 infusions delivered.
Key Statistic: MADRS fell 11.8 points by week 4 (d = 1.2, p < 0.001); music vs no-music: no significant difference on any outcome. Peak MEQ explained adj. R² = 0.356 (MADRS) and 0.489 (BDI) at week 4.